Borderline diabetes, also referred to as prediabetes, is a metabolic condition in which blood sugar levels are elevated but not yet within the range of diagnostic for diabetes. Individuals with borderline diabetes have higher-than-normal blood glucose levels, indicating weakened glucose metabolism. At this stage, it is very critical to know how to control borderline diabetes. As it marks an increased risk of progressing to type 2 diabetes if proactive measures are not taken. Commonly associated with lifestyle factors such as poor diet, lack of physical activity, and excess body weight, prediabetes often presents with no noticeable symptoms. It is a reversible condition, and through lifestyle modifications like adopting a healthy diet, engaging in regular exercise, and maintaining a healthy weight, individuals with borderline diabetes can significantly reduce their risk of developing full-blown diabetes. Regular monitoring of blood sugar levels and consultation with healthcare professionals are essential to managing and preventing the progression of prediabetes. However, there are some major key points related to natural and medical cures involved to help you manage borderline diabetes.
Natural Approaches

Controlling borderline diabetes, or prediabetes, involves lifestyle modifications to improve insulin sensitivity and prevent the progression to type 2 diabetes. To know, how to control diabetes at home? There is a primary approach consists of five natural ways to deal with borderline diabetes including:
1. Healthy Eating Habits
A balanced diet emphasizes whole, nutrient-dense foods, including fruits, vegetables, lean proteins, and whole grains. Healthy eating habits play a pivotal role in controlling diabetes by helping to manage blood sugar levels effectively. It’s essential to monitor carbohydrate intake, opting for complex carbohydrates with a low glycemic index to avoid rapid spikes in blood sugar. Portion control is crucial to prevent overeating and maintain a healthy weight. Limiting the consumption of processed foods, sugary snacks, and sweetened beverages is vital. In addition, incorporating heart-healthy fats, such as those found in avocados, nuts, and olive oil, can contribute to overall well-being. Adopting these healthy eating habits fosters stable blood sugar levels, supports weight management, and contributes to overall diabetes management.
2. Regular Physical Activity
To see, how to control diabetes with exercise? Keep remembering that regular physical activity is a cornerstone in controlling diabetes, playing a pivotal role in managing blood sugar levels and promoting overall health. Engaging in aerobic exercises such as brisk walking, jogging, swimming, or cycling helps improve insulin sensitivity, allowing cells to better respond to insulin and efficiently utilize glucose. Furthermore, incorporating strength training exercises enhances muscle mass, contributing to better glucose metabolism. Physical activity aids in weight management, another key factor in diabetes control. Aim for at least 150 minutes of moderate-intensity aerobic exercise per week, complemented by strength training sessions at least twice a week. Exercise not only helps regulate blood sugar levels but also contributes to improved cardiovascular health and increased energy levels.
3. Stress Management and Adequate Sleep
In managing borderline diabetes, incorporating effective stress management techniques, and ensuring adequate sleep are integral components of a holistic approach. Chronic stress can contribute to elevated blood sugar levels through hormonal imbalances, exacerbating insulin resistance. Implementing stress-reducing practices such as mindfulness, meditation, deep breathing exercises, or engaging in enjoyable activities can positively impact blood glucose control. Moreover, prioritizing adequate and quality sleep is essential, as sleep deprivation can impair insulin sensitivity and lead to hormonal imbalances that may contribute to the progression of prediabetes to full-fledged diabetes. Establishing consistent sleep patterns and creating a relaxing bedtime routine can promote better sleep quality. By addressing both stress and sleep, individuals with borderline diabetes can enhance their overall well-being and contribute to a more comprehensive strategy for diabetes prevention.
4. Maintain a Healthy Weight
Maintaining a healthy weight is a fundamental aspect of controlling borderline diabetes, also known as prediabetes. Excess body weight, particularly around the abdomen, is closely linked to insulin resistance and an increased risk of developing type 2 diabetes. Achieving and sustaining a healthy weight through a combination of balanced nutrition and regular physical activity is crucial. Even modest weight loss, around 5-10% of body weight, can significantly improve insulin sensitivity and reduce the likelihood of progressing to diabetes. Adopting a nutrient-dense diet that is mindful of portion sizes, combined with at least 150 minutes of moderate-intensity aerobic exercise per week and strength training exercises, can support weight management efforts. It’s essential to approach weight loss and maintenance with realistic goals and a long-term perspective, making sustainable lifestyle changes that promote overall health and reduce the risk of diabetes complications.
5. Regular Monitoring and keeping Log
Regular monitoring of blood sugar levels is a crucial component in effectively managing borderline diabetes, also known as prediabetes. Monitoring provides valuable insights into how specific foods, physical activity, and lifestyle choices impact blood glucose levels. This information empowers individuals to make informed decisions about their diet and exercise routines, facilitating better control of blood sugar fluctuations. Self-monitoring with a glucometer or other recommended methods allows for timely adjustments to lifestyle factors and helps track progress in managing prediabetes. Healthcare professionals may also recommend periodic laboratory tests to assess average blood glucose levels over time. Consistent monitoring fosters a proactive approach to diabetes management, enabling individuals to take charge of their health and make necessary adjustments to prevent the progression of type 2 diabetes
Medical Approaches
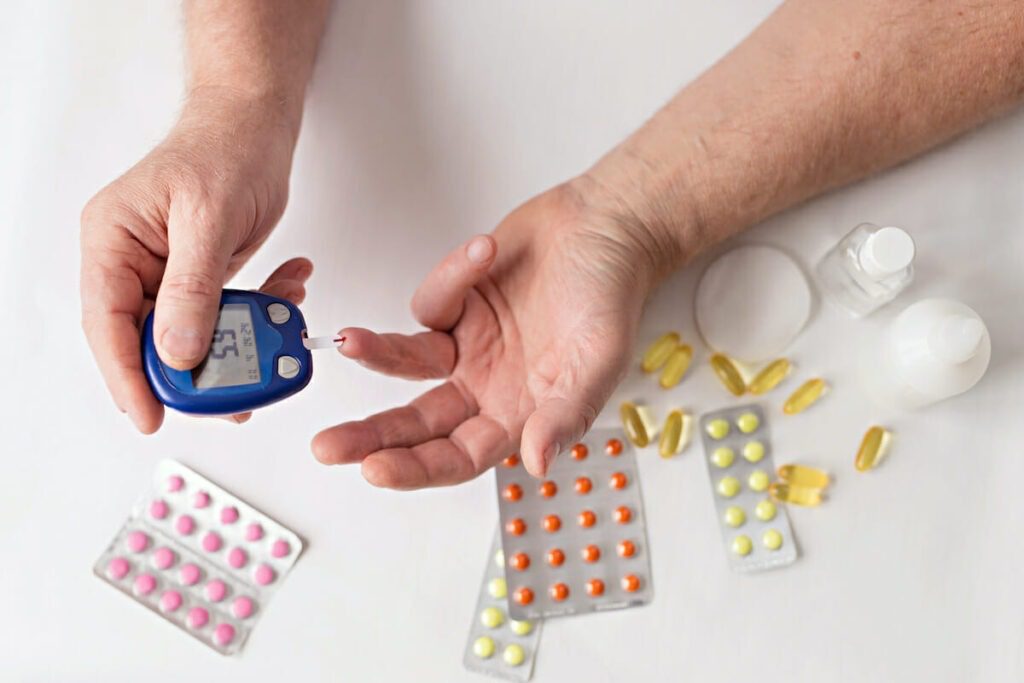
Lifestyle modifications are often the secondary approach directed toward how to control borderline diabetes (prediabetes) medically. Some medications may be prescribed in certain cases. It’s important to note that medication should be used in conjunction with healthy lifestyle changes. Here are five medical strategies that may be employed to control borderline diabetes:
1. Metformin
Metformin, a commonly prescribed medication, plays a significant role in the medical management of borderline diabetes, also known as prediabetes. As a first-line treatment, metformin helps improve insulin sensitivity and reduce glucose production by the liver. By enhancing the body’s response to insulin, metformin assists in regulating blood sugar levels, which is crucial in preventing the progression from prediabetes to type 2 diabetes. It is often prescribed in conjunction with lifestyle modifications such as a balanced diet and regular exercise. Metformin is effective in lowering blood glucose levels and improving overall metabolic health in individuals with prediabetes. However, it is essential to use metformin under the guidance of healthcare professionals, who can determine the appropriate dosage and monitor its effects, considering individual health conditions and potential side effects. Additionally, metformin is usually part of a comprehensive treatment plan that includes regular monitoring, lifestyle changes, and ongoing medical supervision to effectively manage borderline diabetes.
2. Other Medications
In addition to metformin, several other diabetes medications may be considered for the medical management of borderline diabetes or prediabetes. Alpha-glucosidase inhibitors, such as acarbose or miglitol, slow down the digestion of carbohydrates in the intestines, helping to prevent rapid spikes in blood sugar after meals. Thiazolidinediones, like pioglitazone, work by improving insulin sensitivity in peripheral tissues, assisting with glucose uptake. These medications are prescribed based on individual health conditions and considerations, aiming to address specific aspects of glucose metabolism. It’s important to note that the choice of medication may vary depending on factors such as overall health, potential side effects, and individual response to treatment. As with any medication, these should be used under the supervision of healthcare professionals who can tailor the treatment plan to the individual needs of the patient. Regular monitoring and follow-ups are essential to assess the effectiveness of these medications and make necessary adjustments to the treatment plan for optimal management of borderline diabetes.
3. Individualized Treatment Plans
The medical management of borderline diabetes relies on individualized treatment plans tailored to the specific health needs and circumstances of each person. Healthcare professionals work closely with individuals with borderline diabetes to develop a comprehensive strategy that typically includes a combination of lifestyle modifications and, if necessary, medications such as metformin. These treatment plans take into account factors such as age, overall health, and potential side effects of medications. Regular monitoring of blood sugar levels and periodic checkups help assess the effectiveness of the treatment plan, allowing for adjustments as needed. Additionally, healthcare providers may provide guidance on nutrition, physical activity, stress management, and other aspects of daily living to empower individuals in actively managing their condition. The individualized nature of these treatment plans ensures a comprehensive approach that considers the unique circumstances of each person with borderline diabetes, fostering better adherence and improved outcomes.
4. Blood Pressure and Cholesterol Management
Comprehensive medical management of borderline diabetes involves not only addressing blood sugar levels but also prioritizing blood pressure and cholesterol management. Individuals with prediabetes often have an increased risk of cardiovascular complications. Medications to regulate blood pressure, such as ACE inhibitors or angiotensin II receptor blockers, and cholesterol-lowering medications like statins, may be prescribed to mitigate these risks. Controlling blood pressure and cholesterol levels is crucial for reducing the likelihood of cardiovascular events, which individuals with diabetes are at a higher risk for. Regular monitoring, medication adherence, and lifestyle modifications, including a heart-healthy diet and regular exercise, are key components of this multifaceted approach. Establishing individualized treatment plans and undergoing regular checkups are essential for effectively managing blood pressure and cholesterol levels in individuals with borderline diabetes, promoting overall cardiovascular health, and reducing the risk of complications.
5. Constant Healthcare Checkups
Regular healthcare checkups are integral to the medical management of borderline diabetes, providing a proactive and preventive approach to monitor and control the condition. Through routine checkups, healthcare professionals can assess key health indicators, including blood sugar levels, blood pressure, and cholesterol levels. These assessments allow for the early detection of any changes or developments related to diabetes risk, enabling timely interventions. Regular consultations with healthcare providers also facilitate ongoing discussions about lifestyle modifications, medication effectiveness, and potential adjustments to the treatment plan. These checkups play a crucial role in empowering individuals with borderline diabetes to make informed decisions about their health, receive personalized guidance, and actively participate in their diabetes management. By establishing a consistent schedule of healthcare visits, individuals can work collaboratively with their healthcare team to optimize their overall well-being and reduce the risk of progressing from prediabetes to full-fledged diabetes.
To summarize, it’s crucial to note how to control borderline diabetes. An effective management of borderline diabetes, or prediabetes, necessitates a multifaceted approach that combines lifestyle modifications with medical interventions when appropriate. On one hand, adopting a balanced and nutritious diet, engaging in regular physical activity, maintaining a healthy weight, and managing stress contribute significantly to controlling blood sugar levels and reducing the risk of progression to type 2 diabetes. Regular monitoring of blood sugar, along with checkups and consultations with healthcare professionals, helps guide personalized treatment plans and ensures timely adjustments. Other hand, medications like metformin may be recommended in some cases to complement lifestyle changes. Recognizing the individualized nature of prediabetes management is crucial, as it allows for tailored strategies that consider unique health conditions and preferences. By embracing these holistic strategies and strengthening a proactive partnership with healthcare providers, individuals with borderline diabetes can take charge of their health, mitigate risks, and work towards achieving long-term well-being.